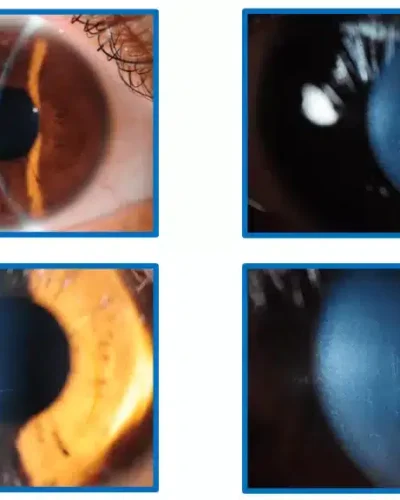
The condition known as keratoconus occurs when the cornea, the transparent, dome-shaped front surface of the eye, thins and eventually swells outward into a cone shape. Blurred vision and possible light and glare sensitivity are caused by a conical cornea.
Environmental and genetic factors are risk factors, but the causes are unknown. About 10% of keratoconus sufferers also have a parent who has the disorder.
To diagnose keratoconus, ophthalmologist will review your medical and family history and conduct an eye exam. Tests to diagnose keratoconus include:
Treatment for keratoconus depends on the severity of condition and how quickly the condition is progressing.
Mild to moderate keratoconus can be treated with eyeglasses or special contact lenses. Patients using rigid or scleral contact lenses need to make sure to have them fitted by an ophthalmologist with experience in treating keratoconus. Patients also need to have regular checkups to determine whether the fitting remains satisfactory.
A process called corneal collagen cross-linking fortifies chemical bonds in the cornea by using UV light and a photosensitiser. The goal of the treatment is to stop ectasia, which is characterised by gradual and asymmetrical changes in corneal shape.
Corneal inserts. (intracorneal ring segments)
improve vision and support the cornea’s shape by flattening the cone.
Corneal inserts can lessen the need for a corneal transplant, restore a more normal corneal shape, and slow the progression of keratoconus. Contact lens fitting and tolerance may also be improved by this procedure. The procedure can be regarded as a temporary measure because the corneal inserts can be taken out if necessary.
Cornea transplant.
Patients will probably require a corneal transplant (keratoplasty) if they have severe thinning or corneal scarring.
A full-thickness corneal transplant is called penetrating keratoplasty. A full-thickness section of your central cornea is removed during this procedure, and donor tissue is used in its place.
The endothelium, the cornea’s inner lining, is preserved during a deep anterior lamellar keratoplasty (DALK). It helps prevent this vital inner lining from being rejected, which can happen with a full-thickness transplant.